Shoulder Arthroscopy
Introduction
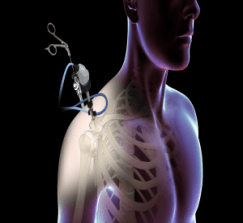
Arthroscopy is a minimally invasive diagnostic and surgical procedure performed for joint problems. Shoulder arthroscopy is performed using a pencil-sized instrument called an Arthroscope. The arthroscope consists of a light system and camera to project images to a computer screen for your surgeon to view the surgical site. Arthroscopy is used to treat disease conditions and injuries involving the bones, cartilage, tendons, ligaments, and muscles of the shoulder joint.
The shoulder joint is made up of a ball and socket joint, where the head of the humerus (upper arm bone) articulates with the socket of the scapula (shoulder blade) called the glenoid. The two articulating surfaces of the bones are covered with cartilage, which prevents friction between the moving bones enabling smooth movement. Tendons and ligaments around the shoulder joint provide strength and stability to the joint. Injury and disease to the bones or soft tissues of the shoulder joint can make it unstable, and lead to pain, inflammation and reduced mobility.
What are the indications for shoulder arthroscopy?
Shoulder arthroscopy is indicated to treat the following shoulder conditions when nonsurgical treatment such as medication and therapy fail to relieve pain and disability:
- Shoulder Impingement: This occurs when the shoulder blade applies pressure on the underlying soft tissues when the arm is lifted.
- Rotator Cuff Tear
- Frozen Shoulder or Adhesive Capsulitis
- Shoulder Instability: This occurs when the head of the upper arm bone slips out of the socket of the shoulder blade’s glenoid cavity either due to injury or overuse
- Biceps Tendonitis or Tear: This occurs when the tendon attaching the bicep muscle to the shoulder become inflamed or tear.
- Damaged Cartilage or Ligaments
- Bone Spurs or Bony Projections
- Arthritis AC Joint
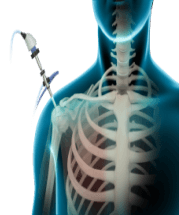
How is the procedure performed?
Your surgeon performs shoulder arthroscopy under general or regional anesthesia. You may be positioned lying down on your side with your arm propped up or sitting in a semi-seated position. Sterile fluid is injected into the shoulder joint to expand the surgical area so your surgeon has a clear view of the damage and room to work. A button-sized hole is made in the shoulder and the arthroscope is inserted. Your surgeon can view images captured by the camera in the arthroscope on a large monitor. Surgical instruments are introduced into the joint through separate small holes to remove and repair the damage to the joint. After surgery, the instruments are removed and the incisions are closed with sutures.
What are the steps taken for post-operative care?
After the surgery, the small surgical wounds take a few days to heal and the surgical dressing is replaced by simple Band-Aids. The recovery time depends on the type and extent of problem for which the procedure was performed. Pain medications are prescribed to keep you comfortable. The arm of the affected shoulder is placed in a sling for a short period as recommended by your doctor. Physical therapy is advised to improve shoulder mobility and strength after the surgery.
What are the advantages of shoulder arthroscopy?
The advantages of arthroscopy compared to open surgery with a large incision include:
- Less pain
- Fewer complications
- Shorter hospital stay
- Faster recovery
- Ability to address concurrent pathology
What are the associated risks and complications?
Complications of shoulder arthroscopy include infection, bleeding, damage to nearby nerves or blood vessels, or delayed healing after the surgery. In certain cases, stiffness of the shoulder joint may occur after the surgery. It is important to participate actively in your physical therapy to prevent this from occurring.
Summary
Shoulder arthroscopy is a minimally invasive surgical procedure used to view the shoulder joint and repair any damage to the bones, muscles, tendons, or ligaments found on observation. It is normally performed on an outpatient basis and is considered more reliable than other diagnostic methods such as X-rays and MRIs.